Public release date: 10-Feb-2011
SAN FRANCISCO (February 10, 2011) — In a study to be presented today at the Society for Maternal- Fetal Medicine’s (SMFM) annual meeting, The Pregnancy Meeting ™, in San Francisco, researchers will present findings that showed that in rats, the use of magnesium sulfate (Mg) significantly reduced the neonatal brain injury associated with maternal inflammation or maternal infection.
Magnesium sulfate is sometimes used during preterm labor to reduce the risk of neonatal brain injury. In 2010 the American College of Obstetricians and Gynecologists and the Society for Maternal-Fetal Medicine issued an opinion that “available evidence suggests that magnesium sulfate given before anticipated preterm birth reduces the risk of cerebral palsy in surviving infants.”
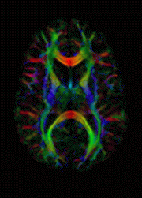
“We knew there were indications from other studies that magnesium sulfate might protect a preterm fetus from cerebral palsy, but we wanted to demonstrate direct and conclusive protective effect on the offspring brain in cases of maternal inflammation” said Ron Beloosesky, M.D., one of the study’s authors. “We wanted to learn more about the protective effects of Mg in cases where maternal inflammation causes preterm birth, so we used the very sensitive diffusion tensor imaging, Magnetic Resonance Imaging to study how Mg works.”
Beloosesky and his colleagues studied pregnant Sprague-Dawley rats at 18 days gestation that received i.p. LPS (500 µg/kg) or saline at time 0. Dams were randomized to treatment with s.c. saline or Mg (270 mg/kg loading followed by 27 mg/kgq20 min) for two hours prior to and following the i.p. LPS or saline. Pups were delivered spontaneously (e21) and allowed to mature until postnatal day 25. Female offspring (4-8 per group) were examined under isoflurane anesthesia by MRI brain imaging and analyzed using voxel based analysis (VBA) after spatial normalization. T2 relaxation time was used to assess for white matter injury and diffusion tensor imaging for Fractional Anisotropy (FA) comparison.
The results showed that offspring of LPS-treated dams exhibited significantly increased T2 levels, and reduced FA levels in white and gray matter (eg, corpus callosum, thalamus, hippocampus), consistent with diffuse cerebral injury. In contrast, offspring of Mg-treated LPS dams demonstrated similar T2 and FA levels as control in both white and gray matter.
The study concluded that Mg treatment significantly reduced evidence of neonatal brain injury associated with maternal LPS. These studies suggest that maternal Mg therapy may be most effective in human preterm deliveries associated with maternal/fetal inflammation.
“The next step, said Beloosesky, “is to do more studies to understand exactly how the Mg works and protects the fetal brain.”
